Prostate Cancer Awareness Month: Why It Matters and How Physical & Occupational Therapy Can Help

September is Prostate Cancer Awareness Month—an important time dedicated to shedding light on one of the most common cancers among those with male bodies. With the goal of enhancing understanding, early detection, and support, this month offers an opportunity to focus on how we can contribute to the fight against prostate cancer, and what to do from a therapy standpoint if you find yourself diagnosed. Whether you’re someone with a prostate or a support person, there are impactful ways to get involved and make a difference.
Understanding Prostate Cancer, Symptoms, and Risk Factors
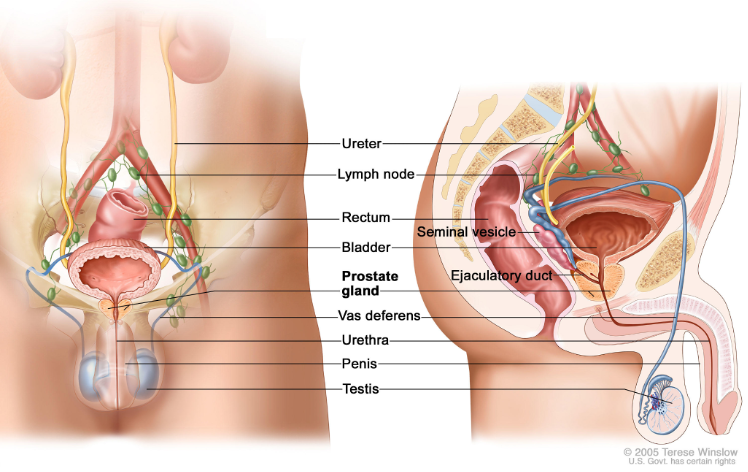
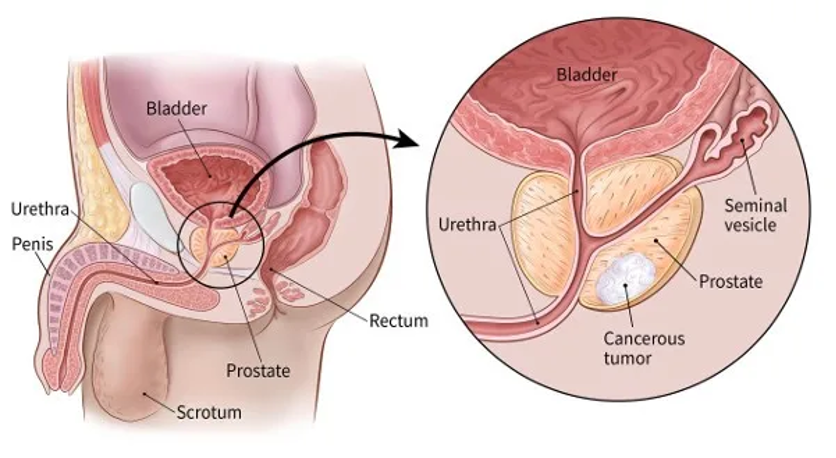
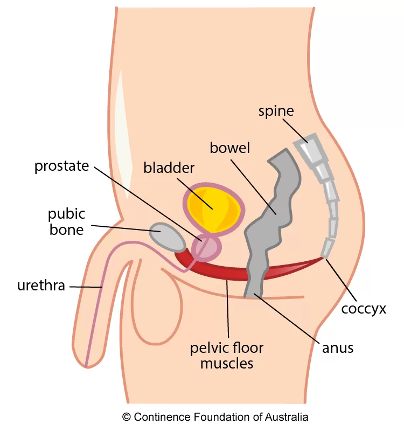
The prostate is a small gland located below the bladder and in front of the rectum that produces semen. Cancer often develops slowly and may not present any symptoms initially, making early detection critical. According to the American Cancer Society, 1 in 8 men will be diagnosed with prostate cancer in their lifetime. The good news is that with early detection and advances in treatment, the survival rates have significantly improved to close to 100% at five years post treatment. Prostate cancer additionally has low chances of spreading, with only 5-7% of those diagnosed having metastasis.
Symptoms
Early prostate cancer often doesn’t cause any symptoms, and most men are diagnosed before symptoms appear. However, these symptoms don’t always mean you have prostate cancer, as many men’s prostates get larger with age due to benign prostate enlargement.
- Urinary symptoms: Frequent urination, especially at night, difficulty starting urination, weak or interrupted urine flow, pain or burning during urination, blood in the urine or semen
- Erectile and ejaculatory symptoms: Difficulty achieving or maintaining an erection, painful ejaculation, blood in the semen
- Pain: Pain in the back, hips, pelvis, chest, or other areas that doesn’t go away
- Other symptoms: Weakness or numbness in the legs or feet, loss of bladder or bowel control, weight loss, feeling very tired
Risk Factors:
- Age: The risk of prostate cancer increases rapidly after age 50, and it’s rare in men under 40.
- Race: Prostate cancer is more common in African American men than in White men.
- Family history: A man’s risk is higher if his father, brother, or son has had prostate cancer.
- Diet: A diet high in fat, red meat, or dairy may increase the risk.
- Obesity: Recent research suggests there may be a link between obesity and prostate cancer.
- Inherited gene mutations: Mutations in the BRCA1, BRCA2, CHEK2, ATM, PALB2, and RAD51 genes may increase the risk of prostate cancer.
- Low levels of selenium: Selenium is a mineral that helps with normal cell function, and low levels in the blood may increase the risk of prostate cancer.
- High levels of vitamin E: The Selenium and Vitamin E Cancer Prevention Trial found that vitamin E taken alone increased the risk of prostate cancer.
- Smoking and chemical exposures
- Inflammation of the prostate
- Sexually transmitted infections
- A balanced diet and regular exercise may lower the risk of developing prostate cancer.
Why Awareness Matters
- Early Detection Saves Lives: Prostate cancer can be asymptomatic in the early stages. Regular screenings, such as PSA (prostate-specific antigen) tests and digital rectal exams, can help detect the disease before it progresses. This screening is vital to begin at age 50, especially if there is a family history of prostate cancer.
- Breaking the Stigma: There’s often a stigma surrounding cancer, particularly with sensitive issues like prostate cancer. Awareness campaigns help normalize conversations about symptoms, treatment options, and coping strategies. This can lead to more men seeking help and getting the care they need.
- Promote Pre and Post Surgical Treatment: Increased awareness leads to greater funding for research and better treatment options. For example, studies have shown that pelvic floor therapy prior to and after surgery will help with lessening side effects! (keep reading for more information)
How Surgery Is Performed
There are several methods for performing a prostatectomy:
- Open Prostatectomy: This is the traditional approach where a large incision is made in the lower abdomen to remove the prostate. This method is less commonly used today due to less invasive techniques available, but it might be necessary in certain cases.
- Laparoscopic Prostatectomy: Also known as minimally invasive surgery, this method involves making several small incisions in the abdomen. A laparoscope (a thin tube with a camera) and other specialized instruments are used to remove the prostate. It usually results in less pain and quicker recovery compared to open surgery.
- Robot-Assisted Laparoscopic Prostatectomy: This is a variation of laparoscopic surgery where a robotic system assists the surgeon. The robot provides greater precision and control through small incisions. It can result in a quicker recovery and fewer complications.
- Transurethral Resection of the Prostate (TURP): This is typically used for treating BPH rather than cancer. A scope is inserted through the urethra (the tube that carries urine out of the body), and the excess prostate tissue is removed. This method doesn’t require an external incision and is less invasive, but it’s not suitable for prostate cancer.
Each method has its own advantages and potential risks, and the choice of technique depends on factors such as the patient’s overall health, the size of the prostate, and the specific condition being treated. Recovery times and outcomes vary, so it’s important for patients to discuss their options thoroughly with their healthcare provider.
Common Side Effects of Prostatectomies
Prostatectomies can have a range of side effects. While individual experiences may vary, here are some common side effects associated with this procedure:
- Urinary Incontinence: This is a common issue where patients have trouble controlling urination. It can range from minor leakage to complete loss of control, often requiring use of protective devices such as liners, pads, or briefs.
- Erectile Dysfunction: Nerve-sparing techniques can help preserve erectile function, but some men may still have trouble achieving or maintaining an erection after surgery.
- Changes in Orgasm: Orgasms might feel different or difficult to achieve after a prostatectomy. Oftentimes, there is a lack of ejaculation, as the prostate and seminal vesicles are removed.
- Lymphedema: If lymph nodes are removed during surgery, there is a risk of developing swelling in the legs or genital area due to lymph fluid buildup.
- Bowel Problems: Some experience changes in bowel habits or discomfort due to the proximity of the prostate to the rectum.
How Physical & Occupational Therapy Can Help
Pelvic floor rehab plays a crucial role in recovery after a prostatectomy, addressing various aspects of post-surgical recovery and helping to improve quality of life. Here are some key ways therapy can help:
- Muscle Strengthening: One of the most common issues following prostate surgery is urinary incontinence. PTs and OTs can work with patients to strengthen the pelvic floor, hip, and abdominal muscles through various exercises. These exercises help improve muscle tone and control, which can reduce leakage and improve bladder function.
- Bladder Retraining: Habit changes can help with urinary frequency and urgency that’s common after surgery.
- Addressing Sexual Health and Function: Prostatectomy can sometimes impact sexual function. Pelvic health therapists can provide guidance on exercises and techniques to support sexual health, as well as address any concerns related to sexual function and intimacy.
- Breathing and Posture: Correct breathing and posture have a direct correlation for optimal pelvic floor functioning!
- Swelling Management: If lymphedema is present, therapists can help address this and improve swelling and any discomfort.
- Education and Support: Physical therapists can educate patients about what to expect during recovery, including how to perform exercises correctly, how to manage any physical limitations, and when to seek further medical help. They can also offer emotional support and encouragement during the recovery process.
Overall, physical and occupational therapy can be a valuable component of a comprehensive rehabilitation plan following a prostatectomy, helping patients recover more effectively and improve their quality of life. Ask your surgeon or primary care provider for a referral to physical or occupational therapy to get started.
How You Can Get Involved
- Educate Yourself and Others: Knowledge is power. Take the time to learn about the risk factors, symptoms, and screening options for prostate cancer. Share this information with friends and family to help increase awareness in your community. Know that pelvic floor rehab is a great option for preventing and treating symptoms after surgery.
- Participate in Awareness Events: Throughout September, numerous events and activities are organized to raise awareness. These can range from local fundraisers and walks to educational seminars and virtual events. Participating in these activities not only helps spread the word, but also supports vital research and patient care initiatives.
- Encourage Regular Screenings: If you’re over 50 or have a family history of prostate cancer, encourage regular screenings. Talk to your healthcare provider about the best screening options for you. For those who are unsure, consulting with a medical professional can provide personalized advice.
- Support Prostate Cancer Organizations: Consider donating to or volunteering with organizations dedicated to prostate cancer research and support. Groups like the Prostate Cancer Foundation and Movember Foundation are at the forefront of advancing research and providing patient support.
- Share Your Story: If you or someone close to you has experienced prostate cancer, sharing your story can be incredibly powerful. Personal accounts can inspire others to take action and provide comfort to those going through similar experiences. Sharing your story also helps create normalcy of symptoms following surgery and can help others seek treatment.
Final Thoughts
Prostate Cancer Awareness Month is about spreading awareness, supporting research, and encouraging early detection so we can make significant strides in the fight against prostate cancer. Whether through education, participation, or support, every effort counts. Let’s come together this September to make a difference and work towards a future where prostate cancer is no longer a major threat to men’s health and treatment is readily accessible if a prostatectomy is necessary.
Stay informed, stay engaged, and let’s keep the conversation going. Together, we can pave the way for better outcomes and brighter futures for all those affected by prostate cancer. Learn more about pelvic health therapy here.
——————————————————————————————————————————-
References:

